 |
| www.strokecamp.org |
 |
| http://www.unitedstrokealliance.org/ |
*****************************************************************
*****************************************************************
While at our Lincoln stroke camp, August 2013, I met Marcia Matthies, Outreach Coordinator for the Nebraska State Stroke Association. She gave me permission to reproduce on our blog any article they have on their site.
This article is packed with information on sleep apnea, and includes many links to even more information.
The following is taken from the Nebraska State Stroke Association web site (www.nebraskastroke.org).
Thank you Marcia
How Healthy Sleep May Prevent Strokes
March 31, 2020
Since stroke is the fifth most common cause of death in the United States, people are eager to find ways to prevent it. Research suggests that sleep health is a major factor related to stroke risk. There is strong evidence that obstructive sleep apnea in particular significantly increases a person’s risk of having a stroke.
This page contains an overview of the many research studies on sleep health and strokes. It also contains information on how to prevent sleep issues that could potentially increase a person’s risk of having a stroke. While the link between sleep health and stroke is not perfectly understood, improving one’s sleep health is beneficial in general, and likely also beneficial in regards to stroke risk.
How Sleep Health Can Cause or Prevent Strokes
Stroke is the fifth leading cause of death in the United States. A stroke happens when a blood clot travels to the brain and blocks a blood vessel, or when a blood vessel in the brain bursts. The following are signs of stroke:
Since stroke is the fifth most common cause of death in the United States, people are eager to find ways to prevent it. Research suggests that sleep health is a major factor related to stroke risk. There is strong evidence that obstructive sleep apnea in particular significantly increases a person’s risk of having a stroke.
This page contains an overview of the many research studies on sleep health and strokes. It also contains information on how to prevent sleep issues that could potentially increase a person’s risk of having a stroke. While the link between sleep health and stroke is not perfectly understood, improving one’s sleep health is beneficial in general, and likely also beneficial in regards to stroke risk.
How Sleep Health Can Cause or Prevent Strokes
Stroke is the fifth leading cause of death in the United States. A stroke happens when a blood clot travels to the brain and blocks a blood vessel, or when a blood vessel in the brain bursts. The following are signs of stroke:
Sudden numbness or weakness, often on one side
Sudden difficulty speaking or understanding
Sudden severe headache
Sudden sight problems
Sudden dizziness or trouble walking
Because strokes can be so deadly and damaging, researchers have been studying how to prevent them for decades. They’ve found many factors that put people at risk for stroke. Some are uncontrollable, such as race, age, the presence of certain genes, and having a low birth weight. Other stroke risk factors include physical inactivity, high cholesterol, high salt intake, high alcohol intake, high blood pressure, obesity, diabetes, cigarette smoking, and more.
Researchers have found that there is a connection between sleep and strokes. The connection between obstructive sleep apnea and strokes is the most well-documented, though there is also a connection between strokes and other sleep disturbances. The following sleep issues are potentially related to strokes:
Obstructive sleep apnea
Central sleep apnea
Insomnia
Restless Leg Syndrome (RLS)
Periodic Limb Movements of Sleep (PLMS)
Sleep loss
Too much sleep
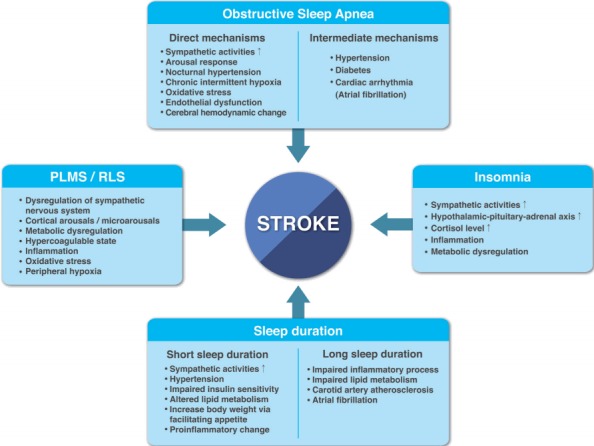
Source: Journal of Stroke
Can Sleep Apnea Cause Strokes?
While researchers do not confirm that there is a direct cause-and-effect relationship between sleep apnea and stroke, they do state that the disorder is an important risk factor for stroke. People who have sleep apnea should take their stroke risk as seriously as those who have high blood pressure or diabetes, or who smoke cigarettes. There are several ways obstructive sleep apnea impacts the body that might explain why it increases stroke risk:
Increased sympathetic nervous system activity
Increased inflammation
Reduced insulin sensitivity
Decreased ability to break down fats
Other cardiovascular and metabolic dysfunction
Researchers recommend that stroke patients undergo a polysomnography, or sleep study, to test for obstructive sleep apnea. Many stroke patients end up having another stroke. Treating obstructive sleep apnea through the use of a CPAP machine may reduce the recurrence of stroke.
A connection between central sleep apnea and strokes has not been confirmed, but central sleep apnea is clearly connected to cardiovascular disease. Cardiovascular problems are closely associated with stroke, so it could be that a clearer link between central sleep apnea and strokes will be found in the future. Anything that negatively impacts the cardiovascular system could potentially increase stroke risk.
One study on obstructive sleep apnea noted that disturbed sleep increases the chance of obesity both directly and by leading to increased food intake and decreased physical activity. Obesity increases the chance of developing obstructive sleep apnea, which along with other factors, increases stroke risk. In this model, disturbed sleep does play a role early on in the path to stroke.
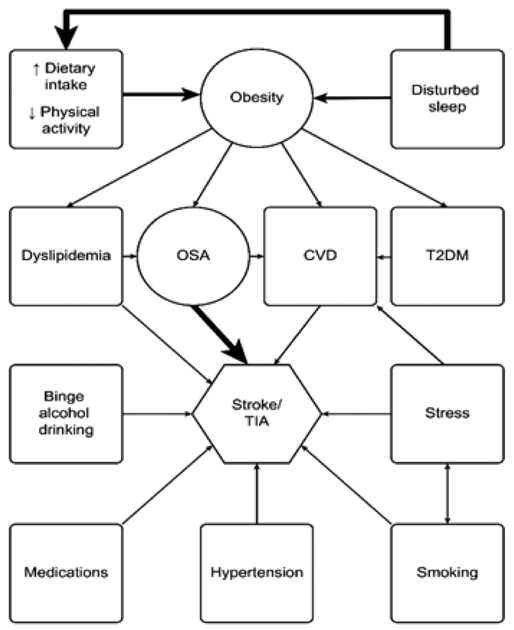
Source: Sleep Medicine and Disorders
Other Sleep Issues and Stroke
Sleep apnea isn’t the only sleep-related issue that increases a person’s chance of stroke. One study showed that non-apnea sleep disorders (NSD) increased stroke risk, particularly in men and the elderly. Non-apnea sleep disorders refers to any sleep disturbance that can’t be attributed to sleep apnea, such as insomnia, sleep disturbance, hypersomnia (too much sleep), disruptions of the 24-hour sleep/wake cycle, sleep-related movement disorders, and any other sleep problems.
Sleep duration is also related to stroke. One study found that both people who sleep less than five hours or over nine hours per night are at an increased risk of dying from stroke or heart attack. This result held true regardless of age, sex, race, smoking status, and body mass index (BMI). While the reason for abnormal sleep duration wasn’t studied, it’s likely that some of the people not obtaining enough sleep have insomnia.
Another study found that people who slept over ten hours per night were more likely to die from cardiovascular problems, including stroke. This could be due to poorer health in those sleeping for longer durations, however.
Studies suggest that movement disorders such as Periodic Limb Movements of Sleep (PLMs) and Restless Leg Syndrome (RLS) are also potentially related to stroke incidence. One study found that more PLMs are associated with White Matter Hyperintensities (WMHs), a blood vessel state that can precede stroke and other cardiovascular issues.
How to Lower the Risk for Stroke With Healthier Sleep
Research demonstrates a connection between sleep issues and strokes. There is strong evidence that having obstructive sleep apnea puts a person at a higher risk for stroke. There is also a clear correlation between sleep duration and stroke incidence, with people who sleep both too little and too much being at greater risk for stroke.
The relationships between stroke and other sleep problems aren’t as certain, though it appears that movement disorders such as Periodic Limb Movements of Sleep (PLMs) could put people at a greater risk of stroke.
Given all of the research on stroke and sleep, people wanting to lower their risk for stroke might consider improving their sleep quality. Anyone suspecting they have a sleep disorder of any kind should consider seeing a sleep specialist and possibly undergo a polysomnography, or sleep study.
Sleep studies and other testing can help doctors determine if a person would benefit from sleep medications or other sleep-related treatments.
Preventing and Treating Sleep Apnea
Sleep apnea is a disorder in which the sleeper has trouble breathing throughout the night. It increases a person’s risk of stroke and is often accompanied by snoring. Here are evidence-based methods for preventing obstructive sleep apnea:
Weight loss in people with obesity
Avoiding the back (supine) sleeping position
Cessation of cigarette smoking
Doctors generally treat sleep apnea by instructing patients to use a CPAP machine, which blows air into the nose and mouth throughout the night. Researchers suspect that CPAP machine use could potentially prevent Transient Ischemic Attacks (TIAs), which are essentially mini-strokes. Their research was preliminary, however, and they recommend larger, controlled studies to determine how well CPAP machines prevent TIAs.
A recent study reported that CPAP machines can reduce the recurrence of stroke and death in patients who have already had a stroke. Other studies show that CPAP machine use decreases blood pressure. This effect is even seen in patients who have high blood pressure that is resistant to treatment.
Since high blood pressure is a risk factor for stroke, CPAP machine use could potentially reduce stroke risk by lowering blood pressure, even in people who have never had a stroke before.
Sleeping for a Healthy Duration
What is considered a healthy amount of sleep depends on a person’s age. People who consistently have trouble sleeping within the healthy range for their age might consider seeing a sleep specialist and undergoing a sleep study. Healthy sleep durations for each age group are as follows:
Newborns: 14 – 17 hours
Infants: 12 – 15 hours
Toddlers: 11 – 14 hours
Preschoolers: 10 – 13 hours
School-Aged Children: 9 – 11 hours
Teenagers: 8 – 10 hours
Adults: 7 – 9 hours
Older Adults: 7 – 8 hours
Sleeping too much or too little is associated with an increased incidence of stroke. There are many different reasons a person might sleep too much or too little, and actions to improve sleep duration will vary depending on the individual. If there is an underlying physical illness or mood disorder affecting a person’s sleep, treating that is important.
If not, there are other actions people can take to help them sleep an ideal amount, such as:
Block out unwanted sound using earplugs or a white noise machine
Avoid drinking excess amounts of alcohol, particularly before bed
Avoid caffeine and other stimulants, particularly before bed
Go to bed and wake up at the same time every day to create a healthy circadian rhythm
Block out light using a sleep mask or blackout curtains
Adhere to a bedtime routine
Preventing and Treating Periodic Limb Movement Disorder
Research shows that Periodic Limb Movement Disorder (PLMD) could contribute to stroke risk. PLMD often overlaps with restless legs syndrome (RLS), narcolepsy, and sleep apnea. The following are ways to prevent and treat PLMD:
Test for other sleep disorders and treat them as necessary
Check medications’ side effects as limb movements can be a result of medications
Test for and treat any other underlying health issues that often accompany PLMD, such as anemia and diabetes
Exercise regularly
Final Thoughts
Sleep issues are one of the many risk factors for stroke, alongside other factors such as obesity, diabetes, cigarette smoking, high cholesterol, high blood pressure, high alcohol intake, high salt intake, physical inactivity, and more. Preventing strokes in individuals and the larger population likely requires a multipronged approach. One strategy for preventing stroke is improving sleep health.
Obstructive sleep apnea is the sleep disorder that has been studied the most in terms of its relationship to stroke. People who have obstructive sleep apnea are at a much higher risk for stroke than people who do not have the sleep disorder.
Central sleep apnea might also contribute to stroke risk since it increases cardiovascular problems. As of now, however, the link between central sleep apnea and stroke risk is not as clearly defined as the link between obstructive sleep apnea and stroke risk.
Other sleep issues beyond apnea appear to also affect a person’s stroke risk. These issues include an abnormal sleep duration, whether that is too much or too little sleep each night, and sleep movement disorders.
Although researchers cannot guarantee that improving sleep will prevent stroke, it is a healthy action worth taking. Early research suggests that CPAP use can reduce stroke risk in people with sleep apnea.
As more sleep-and-stroke-related research is conducted, more connections will likely be found. Pursuing healthy sleep is a worthwhile endeavor anyone, but may have additional benefits for people wanting to prevent stroke.
Additional Resources
If you’re interested in strokes and sleep, these articles might also be of interest to you:
Sleep-Related Breathing Disorders
Obstructive Sleep Apnea
Heart Disease and Sleep
Insomnia
Sleep Health
New Study Finds Sleep Apnea Treatment Can Reduce Hospital Readmissions
























